Cornea Specialists, Surgeons & Doctors
 When you visit the Maine Cornea Specialists at Eyecare Medical Group in Portland you will be pleased to find a group of eye doctors who are experienced specialists in the diagnosis and treatment of all types of cornea disease. The doctors are actively involved in providing patients with a full range of treatment options for corneal disease including corneal transplants such as penetrating keratoplasty, DMEK, DSAEK, and DALK. They are dedicated to delivering friendly, compassionate but professional Cornea care in Portland, Maine.
When you visit the Maine Cornea Specialists at Eyecare Medical Group in Portland you will be pleased to find a group of eye doctors who are experienced specialists in the diagnosis and treatment of all types of cornea disease. The doctors are actively involved in providing patients with a full range of treatment options for corneal disease including corneal transplants such as penetrating keratoplasty, DMEK, DSAEK, and DALK. They are dedicated to delivering friendly, compassionate but professional Cornea care in Portland, Maine.
The Cornea, Corneal Diseases & Surgery
To understand Corneal Diseases and Surgery it is necessary to know about the structure and the functioning of the Cornea. The Cornea is an important structure of the eye that functions in a number of ways to help provide clear vision. It is the clear outermost skin of the eye that acts as a “lens” to focus light rays into the eye. Normally it is about the size and thickness of a dime and is curved in a domed shape. It is critical for the Cornea to maintain its transparency as well as its shape in order to function properly. When light strikes the cornea, it focuses or refracts the incoming light onto the Crystalline Lens of the eye. The Crystalline Lens further focuses that light onto the retina, a layer of light-sensing cells lining the back of the eye. For you to see clearly, light rays must be precisely focused by the Cornea and Crystalline Lens to create a sharp image on the Retina. The Retina absorbs the light rays and sends a signal to the brain where it is interpreted as vision. The Cornea also serves as a filter, screening out some of the most damaging ultraviolet (UV) wavelengths in sunlight. Without this protection, the Lens and the Retina would be highly susceptible to injury from UV radiation. Finally, the Cornea shields the internal structures of the eye from invasion, microorganisms, dust, and debris.
There are a number of eye diseases, conditions or problems that can affect the functioning of the cornea and thus your ability to see clearly. These can include:
- Eye Injuries
- Eye Infections
- Inherited Familial or Genetic Conditions
- Age-Related Changes
It is often possible to treat these conditions with eye drops or other medications, various types of surgery, or contact lenses. Certain conditions may not be resolved with medications and may require corneal replacement or transplantation. At Eyecare Medical Group, Adam Sise, M.D. is a fellowship-trained corneal specialist. This means that in addition to the extensive education and training that he completed becoming an eye surgeon or Ophthalmologist, Dr. Sise completed additional training to provide specialized medical and surgical care to treat corneal disease.
Thus as a Corneal Specialist, Dr. Sise provides consultation, diagnosis, and treatment for the full range of medical and surgical conditions affecting the anterior segment of the eye. These include infections of the cornea, corneal dystrophies, corneal trauma and scarring, cataract, keratoconus, pterygium, and ocular surface tumors.
Corneal Infections
About Corneal Infections
The outermost layer of the Cornea is called the epithelium. If can be damaged from trauma of any type, including a foreign body such as a piece of metal, a poke in the eye from a branch or a finger, or even from a dirty or damaged contact lens. It is then possible for bacteria, viruses or fungi to penetrate the Cornea and cause an infection. An infection of the cornea is called Keratitis or Ulceration. Keratitis can cause a painful inflammation with a discharge, which if not treated quickly and appropriately, can lead to corneal scarring and loss of vision. Corneal scarring results in a loss of corneal transparency and can necessitate corneal transplantation to restore vision. Pain and redness are common in corneal infections, but not all infections are painful.
If Dr. Sise suspects that you have a corneal infection, he will look for certain diagnostic signs to help him decide the best course of treatment. The treatment may include an antibiotic eye drop that acts against the suspected organism and it may also include a steroid eye drop to help reduce the inflammation. Depending on the type of infection suspected, pills may also be prescribed.
Herpes Zoster Keratitis (Shingles)
Herpes Zoster Keratitis is caused by the same virus that causes chickenpox, named Varicella-Zoster Virus. It is thought that the Varicella-Zoster Virus remains in the nerve cells of your body in an inactive state long after having chickenpox earlier in life. The Varicella-Zoster Virus can reactivate later in life and travel through the nerves in your body causing a painful blistering rash. If the Varicella-Zoster Virus travels to your head or neck, it can affect the eye and the cornea.
It is critical to have an Eyecare Medical Group physician diagnose this quickly as the infection can penetrate deeper into the cornea and cause scarring. The infection can also result in a loss of corneal sensation, which can be permanent. Dr. Sise may prescribe both oral medications and eye drops to try and resolve the infection and prevent serious damage from occurring.
It is possible for anyone who has been exposed to the Varicella-Zoster Virus to get shingles, however, it most frequently seems to affect those of advanced age and those with weakened or suppressed immune systems. Further, corneal problems from shingles may occur many months after the facial shingles appear to have resolved. Therefore, if you have had facial shingles it is important for you to schedule an appointment with Dr. Sise.
Ocular Herpes and Herpes Keratitis
Ocular Herpes or Herpes of the eye is caused by the Herpes Simplex Virus and is the most common cause of corneal blindness in the United States today. Up to 50% of people who have a single Herpes Simplex viral infection of the eye will experience a flare-up or recurrence. The virus often leads to irreversible scarring of the cornea.
Ocular Herpes may start as a painful sore on the eyelid or surface of the eye. If left untreated, it may multiply and begin to destroy epithelial cells and progress deeper into the cornea. If the Ocular Herpes penetrates the deeper layers of the cornea and causes a Stromal Keratitis it may cause corneal scarring-so prompt diagnosis and treatment of Ocular Herpes is important.
It is estimated that 400,000 people in the United States have had some type of Ocular Herpes, with more than 50,000 initial and recurring cases being diagnosed each year. Of these, it is believed that 25% is the more severe form of Herpes Stromal Keratitis. The recurrence of Herpes Simplex eye infections is significant in that it appears to recur in about 10% of patients with one year, 23% of patients within two years and 63% of patients within 20 years of their initial infection. Sometimes a recurrence can be prompted by sunlight, stress, fevers or an unrelated eye injury.
Our physicians may prescribe both oral medications and eye drops to try and resolve the infection and prevent serious damage from occurring. Prompt diagnosis and medication is key to preventing any vision loss.
Corneal Dystrophies
Fuchs’ Dystrophy
Fuchs’ Endothelial Dystrophy is a slowly progressive disease of the cornea that is generally found in both eyes and is slightly more common in women than men. While it is possible to observe Fuchs’ Dystrophy in people in their 30’s and 40’s, it usually does not compromise vision until people are in their 50’s or 60’s. The innermost layer of cells in the cornea, called the endothelium, is a single layer of non-regenerating cells. The endothelial cells are responsible for pumping water out of the cornea and helping to maintain corneal transparency and thickness. While the reason is poorly understood, in Fuchs’ Dystrophy, the endothelial cells die prematurely. In the early stages, patients often notice increased glare, especially when driving at night. Later in the condition, the cornea becomes swollen and cloudy which leads to blurred vision. In its most advanced stage, Fuchs’ Dystrophy is associated with episodes of eye pain as the epithelium “blisters” by forming “bullae”, which actually begin to burst open.
Early in the course of Fuchs’ Dystrophy patients will wake up with blurry vision that gets progressively clearer as the day passes. This phenomenon occurs because the cornea normally takes on water and swells during sleep. In Fuchs’ Dystrophy, the endothelium removes fluid from the cornea less efficiently and is unable to keep the cornea clear and compact overnight. Over time, if Fuchs’ Dystrophy worsens and the vision does not clear, Dr. Sise will attempt to reduce the corneal swelling with eye drops and ointments. If these measures fail to provide comfort and clear vision, it may be necessary to have a Corneal Transplant.
For some patients, those patients requiring surgery, a newer procedure is known as DMEK (Descemet’s Membrane Endothelial Keratoplasty) can safely restore vision. Dr. Sise can perform this procedure, which is a type of transplant, to help certain Fuchs’ Dystrophy patients overcome their discomfort and vision loss. In some cases, a descement-stripping procedure may be performed that does not require a transplanted tissue.
Map-Dot-Fingerprint Dystrophy or Anterior Basement Membrane Dystrophy
The outermost layer of the cornea, called the epithelium, is attached or anchored to an underlying basement membrane. In some individuals, the epithelial basement membrane develops abnormally making it difficult or impossible for the epithelium to adhere properly to the basement membrane. This can result in blurry vision and a syndrome known as Recurrent Corneal Erosions. Recurrent Corneal Erosions can be painful and cause the corneal surface to become irregular. This will lead to the intermittent blurry vision along with the discomfort and foreign body sensation. It usually affects adults between the ages of 40-70 but can often begin earlier. Its appearance is subtle and can be easily overlooked during a routine eye examination. As the name implies, the condition is diagnosed by the appearance of opaque dots, and fingerprint-like whorls or lines in the outermost cornea.
Dr. Sise will often discover Map-Dot-Fingerprint Dystrophy during a routine eye examination in patients who do not have any noticeable symptoms. In this case, treatment is not usually required. For symptomatic patients, Dr. Sise may prescribe lubricating eye drops, patch the eye, or apply a soft bandage contact lens. In more severe cases, a procedure to polish the cornea can restore a normal surface.
Corneal Conditions & Problems-Recurrent Erosion & Pterygium
Recurrent Corneal Erosion
Recurrent Corneal Erosion is a condition of the cornea whereby there is a poor attachment of the outermost layer of the cornea, the epithelium, to the underlying basement membrane layer. Patients who experience Recurrent Corneal Erosion may complain of sharp pain, light sensitivity, tearing and watering of their eyes, and a gritty sensation. Often this occurs upon awakening or after rubbing the eyes. Recurrent Corneal Erosion is a condition that may be associated with Map-Dot-Fingerprint Dystrophy. Dr. Sise may initially prescribe an eye ointment at bedtime as the first line of treatment. This medication helps the epithelium to adhere more firmly to the underlying basement membrane. Artificial tears may also be recommended during the day to keep the cornea moist and lubricated. Sometimes, a soft bandage contact lens will be used to help the healing process in a patient with an active erosion. Those patients who have corneal dystrophy may require additional treatment. This can include a procedure where the epithelium is either gently removed, or microscopic “spot welds” are made on the cornea to encourage the epithelial layer to bond securely to Bowman’s Membrane.
Pterygium
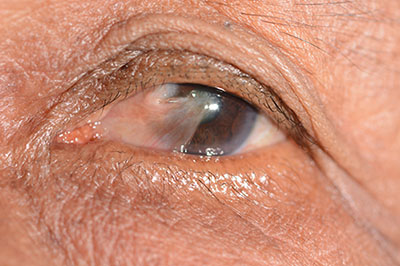 A pterygium is a fleshy triangular growth of tissue on the cornea that may grow slowly throughout a person’s life. Rarely, a pterygium can grow across the cornea and block the pupil. It can also cause blurred vision by increasing astigmatism. People who have been exposed to higher amounts of sunlight and UV radiation are more prone to developing pterygia. Pterygia may become red, swollen and inflamed. Occasionally they need to be removed because of chronic discomfort or to prevent vision loss. Pterygium removal is a surgical procedure that has evolved over time with techniques to prevent the regrowth of the abnormal tissue. As a Corneal Specialist, Dr. Sise uses a surgical technique with conjunctival thin-strip auto-grafting in order to prevent recurrences and obtain the best possible results for Pterygium surgery. In most cases, special tissue glue is used for the best result and no sutures are needed.
A pterygium is a fleshy triangular growth of tissue on the cornea that may grow slowly throughout a person’s life. Rarely, a pterygium can grow across the cornea and block the pupil. It can also cause blurred vision by increasing astigmatism. People who have been exposed to higher amounts of sunlight and UV radiation are more prone to developing pterygia. Pterygia may become red, swollen and inflamed. Occasionally they need to be removed because of chronic discomfort or to prevent vision loss. Pterygium removal is a surgical procedure that has evolved over time with techniques to prevent the regrowth of the abnormal tissue. As a Corneal Specialist, Dr. Sise uses a surgical technique with conjunctival thin-strip auto-grafting in order to prevent recurrences and obtain the best possible results for Pterygium surgery. In most cases, special tissue glue is used for the best result and no sutures are needed.
Corneal Collagen Cross-Linking
Corneal Collagen Cross-Linking is a minimally invasive treatment that may strengthen the cornea and may prevent corneal ectasia or “bulging” in diseases such as keratoconus. The cross-linking treatment is thought to work by forming new bonds within the cornea, which act as stabilizers or anchors. This is thought to stop or slow the bulging often seen in Keratoconus. Corneal Collagen Cross-Linking is performed by placing riboflavin eye drops onto the surface of the eye and exposing the surface to a precise amount of ultraviolet light. Since no other treatment is currently available to prevent the progression of Keratoconus, the FDA approval of Collagen Crosslinking is widely anticipated by many Cornea Specialists.





