Cataract Surgery in Maine
Cataract Surgery Helps Individuals with Aging Eyes

Cataract surgery with lens implantation has become the most common type of surgery performed by medical doctors throughout the world. As advancements in surgical technology and lens implantation options continue to develop, the surgery has become a very good option for many patients as their vision begins to deteriorate in different ways throughout life. We see a significant number of patients each day at Eyecare Medical Group for cataract and lens implantation evaluations; all of whom are seeking improvements in their vision, a reduction in dependence on glasses, and an improvement in their quality of life.
Cataract Surgery: A Straightforward Solution to an Inevitable Problem
When our cataract patients start to notice difficulties with blurred or clouded vision, glare symptoms while driving or in the sunlight, and increased dependence on eyeglasses; we want to encourage them to seek out a solution. When these visual changes begin to interfere with the comfort and safety of one’s daily activities, it is often a great time to consider cataract surgery with lens implantation. An early awareness in the symptoms of cataract, coupled with the knowledge surrounding the safety and benefits of modern-day cataract surgery, allows our patients to safely and effectively overcome, and avoid, the potential limitations that cataract progression will inevitably present.
Our state-of-the-art ambulatory surgery center provides an ideal platform in which the most advanced medical technology and intraoperative equipment are used to safely provide the best and most precise, outcomes for our patients.
Cataracts in Maine
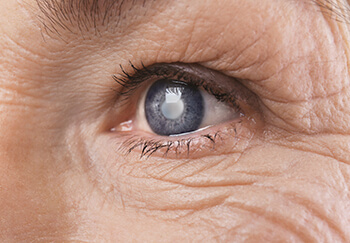
Cataracts are the leading cause of blindness worldwide. About 24 million Americans aged 40 and older have cataracts, and more than half of all Americans develop cataracts by age 80. A cataract is a clouding of the crystalline lens of the eye preventing light rays from passing through it easily. Symptoms of cataracts may include a clouding or blurring of vision, sensitivity to light and glare, double vision or shadowing in one eye, fading or yellowing of colors and poor night vision, sometimes with haloes around lights.
In order to have a good understanding of cataracts, it is important to learn a little about the way your eyes function. Seeing “normally” and having clear vision requires that light be free to pass through the optical structures of your eyes and focus an image on your retina.
In particular, there are two structures that are responsible for refracting, or bending, the light so that it can focus properly. The first important structure is the cornea, which is the outermost clear curved “lens” that is visible when looking at your eye from a side view. The second structure is called the crystalline lens, which is located behind the colored part of the eye, or the iris, and is not directly visible.
The crystalline lens will be examined during your eye examination by using specialized instruments to look through the pupil or the dark center of the iris. Both the cornea and the crystalline lens need to be perfectly clear in order for you to have good vision. If you are in good health and have not had chronic eye infections, inflammation or had any trauma to your eyes, the cornea is likely to maintain its clarity throughout your life. The crystalline lens, however, undergoes a number of changes that progress as we age. These aging changes can affect your vision.
Usually, by about the time we reach the age of 40 years old, most of us begin to experience some of the visual effects that result from changes in the crystalline lens. Even if you have had “good eyes” and “normal vision” all your life, your vision is likely to begin to change in a number of ways. When we are younger, the crystalline lens is usually soft, flexible and “crystal” clear so that it has excellent transparency and optical clarity. As we progress through our 50’s and 60’s, the normally “crystal” clear lens may gradually become yellow and cloudy.
When this occurs, you may initially experience a mild blurring of your vision and feel like you may need a change of eyeglasses. As the crystalline lens continues to lose its transparency and its optical clarity, you may notice that it is not as easy to see well and comfortably in dim illumination, such as for night driving. You may notice that the colors look faded. The cloudiness may also create glare, haloes, light sensitivity and a continuing decrease in your vision. If the crystalline lens becomes too cloudy it may cause a significant decrease in both your day and night vision. These are the visual symptoms you may notice when the crystalline lens has clouded and formed a Cataract.
Cataract Symptoms & Eye Problems
- Blurring or Clouding of Vision
- Glare, or Light Sensitivity
- Poor Night Vision
- Double Vision in One Eye or a Shadowy Image
- Needing Brighter Light to Read
- Fading or Yellowing of Colors


What are Cataract Risk Factors?
Cataract Risk Factors
With people living longer, healthier lives – our knowledge regarding risk factors for cataract development has continued to grow. Patients often ask what they may be able to do to decrease their cataract risk profile. Importantly, age remains the single biggest risk factor contributing to cataract progression as the aging lens in the eye becomes cloudy, rigid, and less effective. However, age isn’t everything…
- Family History – There are a number of different relatively rare genetic conditions that predispose patients to certain types of cataracts. These conditions, and others, can have a hereditary transmission causing cataracts to be more visually significant earlier in life. Be sure to tell your eye doctor if you are aware of someone in your family that was diagnosed or treated for cataract.
- Diabetes – Diabetes has become the number one cause of vision loss in the United States in patients between the ages of 20-75. One of the primary ways in which this condition causes vision loss is through the early development of cataracts. The crystalline lens is highly sensitive to elevated blood glucose and compromised glucose metabolism, as seen with suboptimal control of diabetes.
- Ultraviolet (UV) Light Exposure – Excessive exposure to UV radiation; whether from unprotected outdoor activities, tanning booths, or sunlamps is a known risk factor for cataract development. This is particularly important for our subset of patients in Maine as many people spend a lot of time on the seacoast, outside, or even skiing! Remember to wear UV protection during these activities to minimize your risk of cataract progression.
- Eye Diseases (e.g. glaucoma, uveitis, retinal detachments) – Intraocular disease can accelerate the rate of cataract progression. Inflammatory conditions, such as uveitis, can lead to rapid progression of cataract and can become very visually significant in the setting of uncontrolled intraocular disease. These conditions can be associated with systemic infections and, commonly, with autoimmune conditions. Patients that develop retinal detachments are highly predisposed to cataract formation as up to 90% of patients that have treatment intervention for a retinal detachment will develop a visually significant cataract within 6-12 months.
- Medications- Certain medications, including steroids prescribed for asthma, ocular conditions, allergies, and other systemic conditions are very strong risk factors for the early development of cataracts. Other commonly prescribed medications that have been linked to cataract formation include statins, commonly used for cholesterol.
- Radiation
- Trauma / Injury to the Eye – Any form of trauma near the eye can promote early and rapid cataract formation.
- Smoking – Not only does it cause a tremendous amount of cardiovascular disease, but cigarette smoking also dramatically increases the risk of cataract. There is a direct relationship between cigarette smoking and visually significant cataract changes; this argues for early smoking cessation or avoidance altogether!
What is Cataract Surgery?
Cataract surgery is safe, effective, and quite common. In the United States, more than 2.5 million people have cataract surgery each year. Thanks to our modern outpatient surgical techniques and advanced technology lens implants, cataract surgery is not only one of the most frequently performed surgical procedures in the United States, but it is also one of the safest and most successful surgical procedures that we can provide to help restore your vision and active lifestyle.
Eyecare Medical Group cataract surgeons will typically perform your cataract operation at our AAAHC certified, Medicare & State of Maine licensed ambulatory outpatient eye surgery center. The Eyecare Medical Group eye surgery center allows cataract patients to have their cataract surgery as well as other types of eye surgery, in a convenient, friendly and cost-effective setting in Portland. Cataract surgery today is quite comfortable. When you arrive at the surgery center there will be a number of staff members present to assist you and make your experience pleasant. The entire process usually only requires a few hours of your time from beginning to end.
Cataract Surgery Procedure & Experience
The cataract surgery procedure at EMG will begin with a few sets of drops being placed in your eye to dilate your pupil. Your eye will then be treated with an anesthetic so that you will feel little if anything during your surgery. Some patients experience pressure, cold or mild burning, but almost never discomfort.
Next, your cataract surgeon will make a very small incision at the outermost edge of your cornea. This incision will be just large enough to allow a microscopic instrument the size of a pen tip to pass through it.
Then, your eye surgeon will gently pass a microscopic instrument through the tiny incision and create an opening in the capsule of the crystalline lens to allow access to the cloudy lens material.
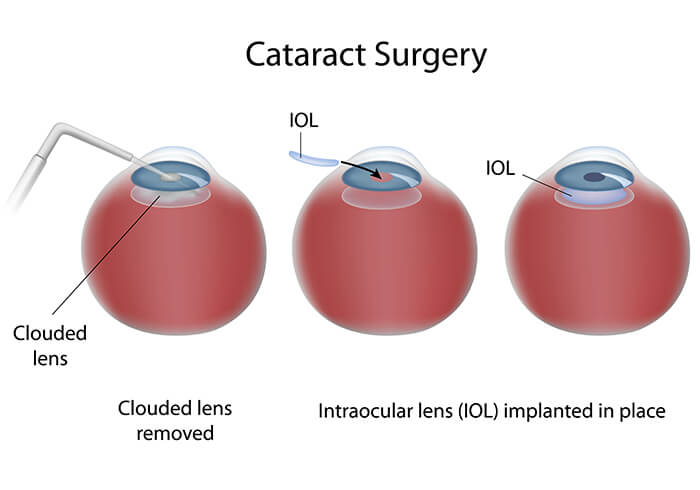
Your eye surgeon will gently pass another sophisticated microscopic instrument through the tiny incision. Sound waves or “Ultrasound” produced at the tip of the instrument will be used to gently break the cataract into pieces small enough to be washed away, drawn through the instrument and removed from your eye. This cataract removal technique is called “phacoemulsification” and is preferred for most patients.
After the cataract has been removed, your cataract surgeon will be able to insert a new, crystal clear permanent intraocular lens implant (IOL) into your eye. The replacement lens will actually be inserted and placed in the correct position through the same tiny incision at the outer edge of the cornea through which the surgeon removed the cataract.
Upon completion of your cataract and lens implant surgery, your surgeon will have one of the surgery center staff members take you to a comfortable place where you will be able to rest and relax prior to going home. After resting for a short while, a surgery staff member will give you permission to have a family member or friend drive you home.
Your surgeon will arrange to see you the next day after your cataract and lens implant surgery so he can examine you in order to confirm that you are healing and seeing as planned. The doctor will also prescribe some eye drops for you to use and may ask you to wear a protective shield, mainly at night, to remind you not to accidentally rub your eye. Although each patient will heal a little bit differently, the majority of patients having cataract surgery at Eyecare Medical Group are able to see well enough to return to their routine daily activities within a day or so after their cataract surgery.
An Important Note about Cataract Surgery
A significant number of men in their 50’s and older experience an enlarged prostate as part of the aging process. Today, many men are taking the prescription medication Flomax® or other similar medications that are members of the class of drugs called “alpha-antagonists” or “alpha-blockers”. These may include Hytrin® (terazosin), Cardura (doxazosin), Flomax® (tamsulosin), Uroxatral® (alfuzosin) and Rapaflo® (silodosin). IT IS VERY IMPORTANT THAT YOU NOTIFY OUR STAFF BEFORE YOU HAVE CATARACT SURGERY IF YOU ARE TAKING ANY MEDICATION FOR AN ENLARGED PROSTATE. Certain medications commonly used to treat an enlarged prostate can cause abnormal movement of muscles controlling the opening and closing of the Iris. During cataract surgery, the pupil must stay enlarged or dilated to allow your cataract surgeon to easily view the Crystalline Lens. Flomax® and certain other alpha-blockers including Hytrin®, Cardura and Uroxatral®, in particular, can interfere with pupil dilation, creating a condition known as Intraoperative Floppy Iris Syndrome (IFIS). If you are taking one of these medications and alert any member of our staff, the EMG cataract surgeons will be able to take extra care to make sure the pupil stays dilated to prevent unexpected complications during your cataract surgery.
What is Cataract Surgery like?
Cataract Surgery Expectations & Recovery
Outstanding medical care is only part of what you’ll experience at our ambulatory surgery center at Eyecare Medical Group. Our experienced staff, with over 200 combined years of nursing experience, is very sensitive to your comfort and take pride in the quality of your patient experience. Knowing what to expect on the day of surgery as well as during your recovery can go a long way toward setting your mind at ease.
The Day of Surgery

Enter through the Surgical Center (rear side of the building) and come inside to our waiting room. Once you’ve checked in with the receptionist, a registered nurse will accompany you to our pre-op area and prepare you for your surgery by reviewing your medical history, your medications, and checking your vital signs. Your nurse will also administer your eye drops. Depending on your procedure, these eye drops could deliver anesthesia, antibiotics, or promote dilation of the pupil in the operative eye.
You’ll then meet our anesthesia team. We have a number of Certified Registered Nurse Anesthetists (CRNAs) to help care for you throughout your surgery experience. They will interview you and explain their role in keeping you comfortable throughout your procedure. An IV will be administered while in the pre-op area to allow the administration of sedatives or other medications that may be required during your surgery.
You’ll receive a gown to put on over your clothes, a hair cover, and booties. A nurse will walk you into the OR which will already be set up for your procedure. Our team will position you comfortably on a bed and cover you with a warm blanket.
You’ll be given medication that makes you relaxed, comfortable, and forgetful. Our caregivers will be monitoring your vital signs throughout the procedure. You’ll wear an automatic blood pressure cuff on your arm, be connected to a heart monitor, and have a clip on your finger to monitor oxygen levels. Your physician will have predetermined what type of anesthesia is best for you and our anesthesia providers will administer one of two types of anesthesia: topical or eye block.
Topical: You’ll receive a sedative through an IV, anesthetic eye drops will be given, and an anesthetic will be administered into the eye at the start of the surgery.
Eye Block: The patient receives a sedative through an IV and a local anesthetic is injected in two places near the eye.
A nurse will then wash around your eye to prepare the area for surgery and sterile drapes will be placed around the surgical area. Once the equipment and lens implant are reviewed and confirmed, everything will be ready for your surgeon to proceed.
You’ll feel safe and cared for throughout the procedure; in fact, one of our caregivers will hold your hand during the surgery. Your surgeon will speak to you from time to time and we will continue to focus on your comfort until the procedure is completed.
After surgery your eye will be cleaned, medication eye drops will be given, and your bed will be raised to a seated position. When you’re ready, your nurse will take you back to the post-op area where we will continue to monitor vital signs. At this time, a friend or family member will be allowed to meet you.
We will review your post-op instructions for the evening and confirm your follow up appointment with your surgeon. We will review what you should expect from your vision and review what types of restrictions and precautions you should follow during your recovery. You will have all the information and contact information necessary should you wish to speak with a surgeon. Your nurse will remove the IV and you’ll be able to leave the surgery center. It is required that someone else takes you home following your surgery.
The Day After Surgery
The next day you’ll come to your doctor’s office for a post-op visit. After a thorough check-up, your doctor will offer more post-op instructions and review medications as necessary.
You’re on your way to a full recovery! We are happy to be a part of that recovery and will work hard to ensure your continued eye health!





